Serpent solutions

23rd February 2024
Sakthi Vaiyapuri FRSB explores how a new generation of antivenoms, alongside better education and more attention, could help reduce snakebite-related deaths
For over a billion people everyday tasks such as walking to school, fetching water or even going to the toilet come with the risk of encountering a venomous snake. A misplaced step or brief lapse in concentration can be fatal.
Venomous and non-venomous snakes can be found in almost all tropical and subtropical countries, and the urbanisation of rural areas and development of land for farming is increasingly encroaching on snakes’ habitats, forcing them into conflict with humans. Although snakes use their venom for predation, and only bite in self-defence as a last resort, more snake–human conflict means more snakebites, including from venomous snakes.
Despite the fact that snakebites have been a health hazard throughout human history, and pose a significant threat to rural, tribal and suburban populations in various parts of the world, snakebite envenoming, or SBE (that is, a snakebite with the injection of venom) was classified as a “high-priority neglected tropical disease” by the World Health Organization (WHO) in 2017.
It has been estimated that around 5.4 million snakebites occur worldwide every year, resulting in 2.7 million envenomings, leading to around 140,000 deaths and 400,000 permanent disabilities every year. That’s almost 7,400 people bitten every day, of whom 200 to 300 will die.
 The development of land for farming is increasingly encroaching on snakes’ habitats, forcing them into conflict with humans
The development of land for farming is increasingly encroaching on snakes’ habitats, forcing them into conflict with humansMost bites occur in remote rural areas, where medical facilities to treat SBE may not be readily available. Further, victims often seek treatments from local healers or take home remedies. A significant number of people die while travelling to distant tertiary healthcare facilities.
Many rural cases never get reported to health authorities and therefore are not counted in SBE statistics. The lack of reliable statistics, and the dangers associated with working with venomous snakes and venoms, has meant SBE has been neglected by health authorities and underfunded for a long time.
India has been identified as the capital of SBE due to its high number of SBE incidences, deaths and disabilities (around 58,000 deaths per year). Here, snakes play a key role in many ecosystems and in controlling insect and rodent populations, and so the eradication of snakes can have cascading impacts on biodiversity and crop yields. Humans need to learn to live with snakes by mitigating the conflicts and seeking prompt treatment when bites occur.
The composition of venom is highly variable, with significant differences observed in the mechanisms of action of different toxins. Venom can induce local tissue damage, coagulopathies, neurotoxicity, myotoxicity and cardiovascular disturbances, or symptoms such as acute pain, swelling, local tissue discolouration, dizziness, nausea, vomiting, sweating, respiratory distress and paralysis.
The severity of effects depends on various factors such as the amount of venom injected, the bite site and the individual’s body mass. There is also variability in the composition of venom in the males, females juveniles, adults or different geographical populations of the same snake species. This all results in highly variable clinical manifestations, which makes diagnosis and treatment difficult.
The problem with antivenoms
New treatments for snakebite are desperately needed. Currently, the only scientifically validated treatment available for SBE is ‘antivenom’, which is made by exposing horses or other large animals including sheep and goats to selected snake venoms and allowing an immune response to occur.
Blood can then be taken from the animals and centrifuged to collect the antibodies for the development of antivenom. It is available mostly in polyvalent form, meaning that it contains a mixture of antibodies against the venoms of a few medically important species. In some countries, monovalent antivenoms may be available against one particular snake venom.
Due to the source of the antibodies, these antivenoms can induce allergic reactions in the patient. The efficacy of the treatments is also dependent on how closely the pool of venoms used for inoculations is related to the venom of the offending snake.
Antivenom can be expensive to produce, has a short shelf life and often requires refrigeration and administration by a trained medical professional. For these reasons, a range of new therapeutic options are being explored to help mitigate the effects of SBE in a cost-effective manner that can be administered in rural low-resource communities where the risk of SBE is greatest.
Existing molecules
Small molecule inhibitors or repurposed drugs are emerging as candidates for the treatment of SBE, as many of these molecules inhibit the toxic actions of key enzymes within the venom.
For example, varespladib, a phospholipase A2 inhibitor, was initially developed to treat patients with acute coronary syndrome, but the drug failed in clinical trials due to the side-effects of long-term use. It is currently in clinical trials to assess its effectiveness in mitigating the systemic and localised effects of phospholipase A2, which is found within the venoms of several snake species.
Animal studies suggest that varespladib inhibits the catalytic activity of this toxin, which promotes cell lysis in bite victims, improving survival rates and decreasing localised damage. A combination of antivenom and varespladib appears to be producing promising results.
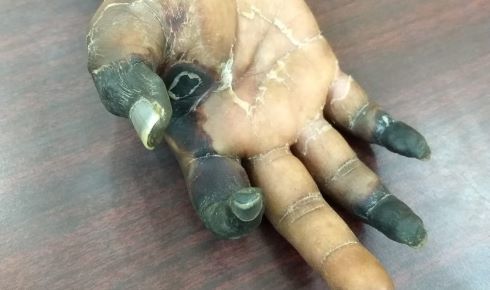 Gangrene following a Russell’s viper bite
Gangrene following a Russell’s viper biteHowever, this inhibitor is specific to only one component found within snake venoms and does not reduce the toxicities associated with other components of the venom. Therefore, combining varespladib with other small molecule inhibitors for other major enzymatic components of venom, such as metalloproteases and serine proteases, could result in the development of a combinational therapy to neutralise the many toxic components of snake venoms.
However, due to the lack of funding for neglected tropical diseases, this research is still in its early stages and is a long way away from being a reality.
Improving antibodies
Another advancing front in snakebite treatment is humanised recombinant toxin-specific antibodies. This approach has the potential to lower antivenom production costs, improve efficacy and decrease the risk of anaphylaxis.
Rather than inoculating animals with venom, recombinant antibodies are produced by identifying the antibody sequence, inserting it into the genome of a cell and culturing the cell to express the antibody. This process can be efficiently expanded to produce antibodies in large quantities without requiring any animal hosts or even the venoms.
The process can use either a ‘top-down’ or ‘bottom-up’ approach. The top-down approach uses recombinant DNA technology to produce a pool of polyclonal antibodies of unknown composition that act on different components of the venom, like the polyclonal antivenoms made in animal serums.
The bottom-up approach produces a narrower pool of antibodies that have been identified as being able to neutralise selected toxins within the venom. This reduces the number of antibodies within the pool, specifically targeting harmful toxins rather than all the components found within the venom.
In the top-down approach, polyclonal recombinant antibodies can be made quickly in large quantities but are likely to have a bias towards the toxins that induce an immune response rather than those inducing damage. The bottom-up approach produces a more efficacious antivenom, but requires a deeper understanding of the toxins within venoms that induce harmful effects.
Alpaca antivenoms
The unique physiology of camelids, such as alpacas and llamas, offers another promising avenue for producing antivenoms. While existing animal-derived antivenoms require refrigeration and suffer from poor stability, camelid antibodies have excellent heat resistance.
Camelid antivenoms are made in the same way as equine antivenoms but the antibodies produced are smaller. This reduces the chances of initiating an immune response and an allergic reaction in patients.
Conventional antivenoms are good at treating systemic envenomation symptoms but not local tissue damage. This is partly due to the large antibodies being unable to pass through smaller or damaged vasculature surrounding the bite site.
The smaller size of camelid antibodies could result in improved neutralisation of venom within tissues, neutralising venom components that stay localised to the bite site, and decreasing the chances of long-term muscle damage and disabilities.
 Awareness and education is also key in reducing the number of deaths from snakebite.
Awareness and education is also key in reducing the number of deaths from snakebite. In low-income tropical countries, camelid antivenoms offer a great advantage as refrigeration may no longer be required, lowering the costs of storing and transporting them in remote areas, which often have poor infrastructure.
Decreasing the amount of time it takes for a victim to reach proper antivenom provision can mean the difference between life and death, and will significantly improve the victim’s chances of surviving without long-term consequences. Camelid antivenoms are still in the early stages of development, with preclinical trials under way to determine their efficacy.
Knowlege is power
With new treatments still a long way from availability and widespread use, education on the risks and proper management of SBE is necessary from a young age to ensure that people are appropriately prepared when they come across a snake and know what to do if they are bitten. Rigorous community health education is critical, particularly in rural communities.
The WHO has developed a strategic roadmap to reduce SBE-induced deaths and disabilities by 50% by 2030. This sets out its ambition for a coordinated, multi-sector effort to improve education, first aid and medical treatment of snakebites.
The clinical management of SBE also needs to be taught for medical and paramedical students, and they should be trained appropriately to handle SBE, which is a complicated issue. Overall, better education, awareness, prompt actions and next-generation antivenoms will significantly reduce the burden of snakebites, and resulting deaths and disabilities.
These simple steps are recommended for immediate SBE first aid and can help reduce the chances of being bitten in the first place
• Keep the home and surrounding area clear of food waste to reduce the number of prey animals that attract snakes.
• Ensure doors and windows are closed when not in use.
• Use a torch to illuminate paths at night and wear closed shoes.
• Snakes only use venom when they feel threatened. If you come across a snake, keep back and give it space.
• All bites from venomous snakes should be regarded as being an envenomation and emergency medical treatment should be sought without any delay.
• The victim should calmly move away from the snake to avoid another bite.
• Traditional remedies and healers do not neutralise the effects of the venom but can delay patients from receiving appropriate medical treatment.
• Keep the appearance of the snake in mind as this might help the doctors to identify whether it is a venomous or non-venomous snake.
• Reassure the snakebite victim and try to prevent any unnecessary movement to avoid the venom spreading.
• Tight jewellery or clothes around the bite site should be removed to prevent the risk of swelling and tissue damage.
• Keep the victim in the recovery position and immobilise the bite site.
• Do not cut or suck the bite site or apply plant extracts, calcium carbonate or any other similar methods, as these are associated with more risks, including infection.
Sakthivel Vaiyapuri FRSB is professor of cardiovascular and venom pharmacology at the University of Reading. With thanks to Jarred Williams and Mr Gnaneswar at the University of Reading and Dr Senthilkumaran at the Manian Medical Centre.


